The Numbers That Matter
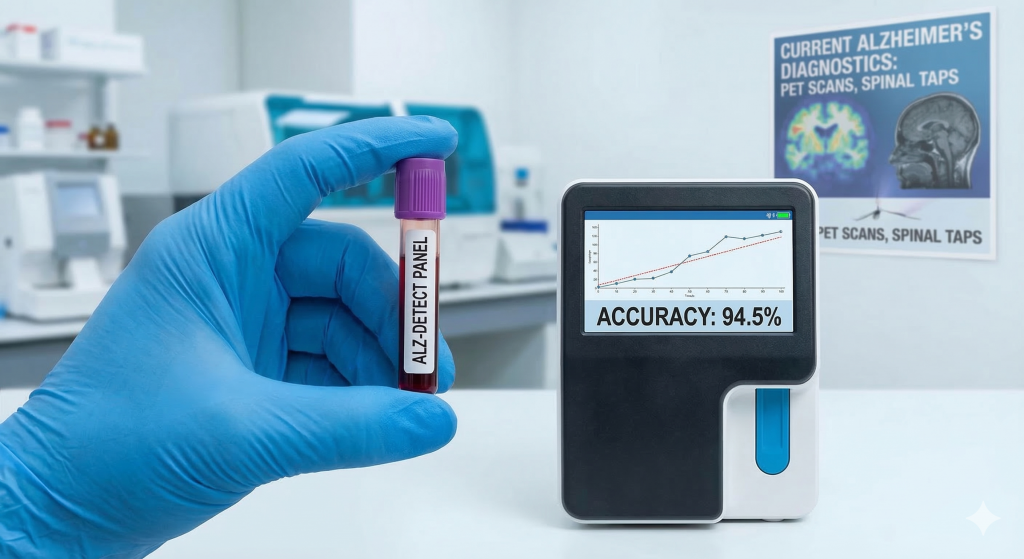
Here’s the thing about medical breakthroughs – they’re usually incremental improvements that get hyped beyond belief. But this blood test study genuinely caught my attention because 94.5% accuracy isn’t just good, it’s revolutionary for Alzheimer’s diagnosis.
Currently, definitively diagnosing Alzheimer’s requires expensive PET scans that can cost thousands of dollars, or invasive spinal taps that many patients understandably want to avoid. The alternative? Doctors make educated guesses based on cognitive tests and family history, which is frustratingly imprecise for something this serious.
What’s interesting here is that this blood test appears to detect specific protein markers that correlate with the brain changes we see in Alzheimer’s. I think the real game-changer is the accessibility – a simple blood draw versus scheduling specialized brain imaging or lumbar punctures.
The study’s methodology seems solid from what I’ve seen, though I’m always cautious about single studies. Still, 94.5% accuracy puts this test in the same ballpark as some of our best diagnostic tools for other major diseases.
Why This Changes the Game for Families

I’ve covered healthcare tech for over a decade, and one thing that consistently breaks my heart is hearing from families stuck in diagnostic limbo. They know something’s wrong, but getting concrete answers about Alzheimer’s has been an expensive, time-consuming nightmare.
This blood test could democratize early detection in a way we haven’t seen before. Think about it – your family doctor could order this test during a routine checkup if there are memory concerns. No specialist referrals, no insurance battles over expensive brain scans, no waiting months for appointments.
Early detection matters enormously because the few treatments we have for Alzheimer’s work best when started early. Plus, families get time to plan, make legal arrangements, and honestly just process what’s coming. That’s invaluable.
The psychological impact can’t be understated either. Right now, many people live with years of uncertainty, wondering if every forgotten name or misplaced key is the beginning of something terrible. A reliable blood test could either provide reassurance or confirm suspicions quickly.
The Business Side Gets Interesting
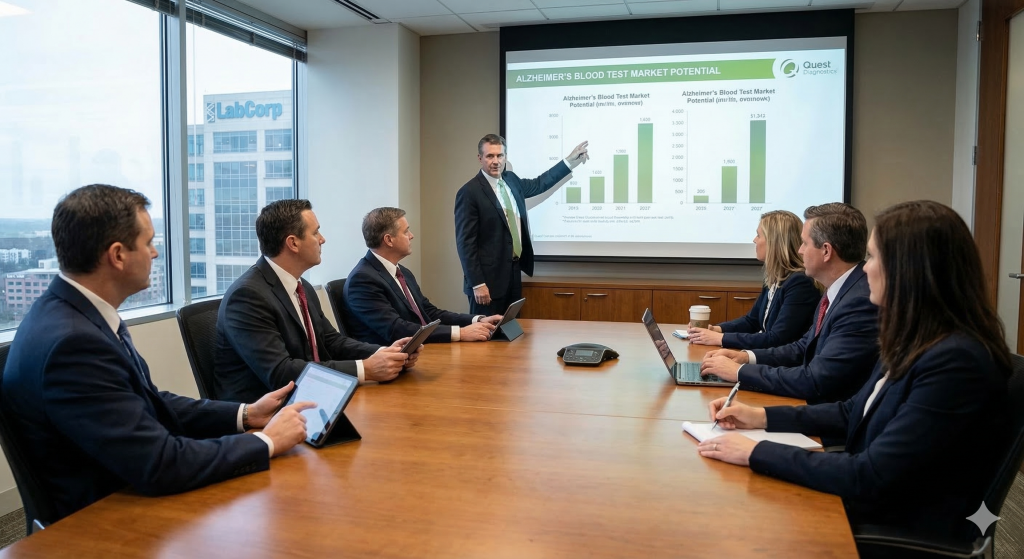
From an industry perspective, this could absolutely reshape the diagnostic landscape. Companies like Quest Diagnostics and LabCorp are probably already calculating how many millions of Americans would want this test annually. The market potential is staggering.
What’s particularly interesting is how this might disrupt the established players in Alzheimer’s diagnostics. Companies making PET scan equipment and specialized brain imaging tech might see demand drop significantly if blood tests become the standard screening tool.
I think we’re also looking at potential integration with existing health tech ecosystems. Imagine Apple Health or other wellness platforms incorporating these biomarkers into broader health tracking. The data possibilities are fascinating, though obviously privacy concerns will be massive.
The pharmaceutical industry is probably the most excited here. Better diagnostic tools mean better clinical trials, faster drug development, and the ability to identify patients who’d benefit most from treatments. This could accelerate Alzheimer’s research significantly.
What Happens Next
Here’s where things get tricky – clinical studies are one thing, but real-world implementation is entirely different. We need FDA approval, insurance coverage decisions, and widespread physician adoption. That timeline could be anywhere from two to five years, realistically.
I’m curious about the cost structure once this hits the market. Will it be positioned as a premium diagnostic tool or priced for mass adoption? That decision will determine whether this becomes a game-changer or just another expensive option for wealthy patients.
The regulatory pathway will be fascinating to watch. The FDA has been increasingly supportive of innovative diagnostic tools, especially for conditions like Alzheimer’s where current options are limited. But they’ll want extensive validation data before approval.
What excites me most is the precedent this sets for blood-based diagnostics. If we can reliably detect Alzheimer’s from a blood sample, what other neurological conditions might be next? We could be looking at the beginning of a revolution in how we diagnose and monitor brain health.
This blood test represents more than just a diagnostic improvement – it’s potentially the key to unlocking earlier intervention, better research, and hope for millions of families. While we’re still years away from widespread availability, the trajectory is clear: simple, accurate, accessible Alzheimer’s diagnosis is finally within reach.